Benefits Leaders Believe in Power of AI, Considering Data Privacy and Accuracy
- None.
- None.
New study indicates that benefits professionals are in an ‘early adopter’ stage with AI
DRAPER, Utah, April 04, 2024 (GLOBE NEWSWIRE) -- HealthEquity, Inc. (Nasdaq: HQY) ("HealthEquity") released the findings of a new survey on Artificial Intelligence (AI) in benefits administration. The survey provides a benchmark on senior benefit leaders’ attitude toward AI-enabled benefits tools.
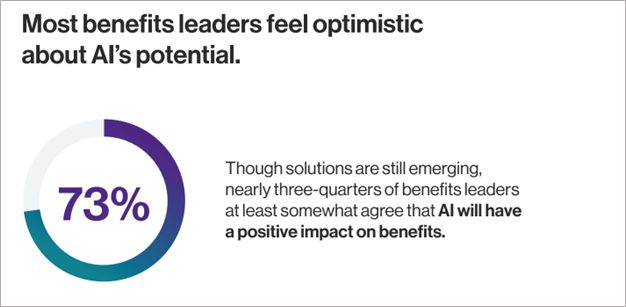
A majority (
"Benefits leaders, like many professionals are learning about what these new technologies can do and they’re optimistic, but they’re also realistic," said Shuki Licht, vice president of Innovation at HealthEquity. “Consumer-facing AI products have opened the door to creating better member outcomes, one that we’re excited about is simplifying the claims process. It’s an exciting time but it’s important that companies using AI are transparent so everyone can feel confident about the results.”
Conducted in February, the survey was administered via Qualtrics to a pool of Directors and VPs of Total Rewards to better understand benefit leader AI perspectives. Additional findings included:
- High belief, high adoption — of those who agreed that AI will have a positive impact on benefits administration,
85% indicated they'd be likely to select a vendor using AI, nearly twice as likely as those who only somewhat agreed. - Reasons to adopt — respondents said improving benefits effectiveness (
38% ) and saving time (29% ) were the main reasons they would work with a partner that incorporates AI. - They want it all — recommending health plans, improving member access to care, model optimal plan design, automation and streamlining claims were seen as areas that would have the most AI impact opportunity in benefits administration.
- Hesitations on privacy and security — respondents said their biggest concern regarding AI was data security and accuracy (
56% ).
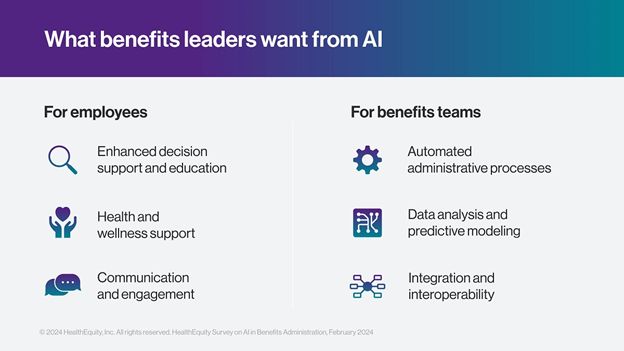
“These results will help the industry to better understand the places to build, and where to tread cautiously with new AI technology," said Jess Cloud, vice president of IT Operations and Transformation at HealthEquity. "We’re going to be strategic with our use of AI insights to drive macro-level improvements at HealthEquity, while protecting our members. Our aim is to utilize the technology to reduce friction points and save time, two areas that are always challenging in the US healthcare system."
Survey results, further insights and recommendations can be found on the HealthEquity Remark blog.
About HealthEquity
HealthEquity and its subsidiaries administer Health Savings Accounts (HSAs) and various other consumer-directed benefits for over 15 million accounts, working in close partnership with employers, benefits advisors, and health and retirement plan providers who share our unwavering commitment to save and improve lives by empowering consumer healthcare. Through cutting-edge solutions, innovation, and a relentless focus on improving health outcomes, we empower individuals to take control of their healthcare journey while ultimately enhancing their overall well-being. Learn more about our “Purple service” and approach at www.healthequity.com
Media Contact:
Amy Cerny
Director of Corporate Communications
acerny@healthequity.com
A photo accompanying this announcement is available at https://www.globenewswire.com/NewsRoom/AttachmentNg/7764cdc5-ba98-4e43-975c-2090126e8a1e
A photo accompanying this announcement is available at https://www.globenewswire.com/NewsRoom/AttachmentNg/54f86024-ae7f-478f-a58a-31ae5d93227a

FAQ
What did HealthEquity, Inc. (HQY) reveal in the new survey?
How many respondents were surveyed in the study?
What percentage of respondents believe AI will have a positive influence on benefits administration?







